She was 36. Healthy, she thought.
Her first pregnancy ended with an emergency: preeclampsia, early delivery, and both survived.
At her postpartum visit, her pressure was still elevated. Her doctor said: Follow up with primary care.
She did not have a primary care doctor. She was 36.
Nobody checked her cholesterol. Nobody connected her pregnancy to her heart.
She found out at 46, after her first cardiac event.
This is a composite story. It plays out thousands of times a year, in exam rooms where the right question was never asked.
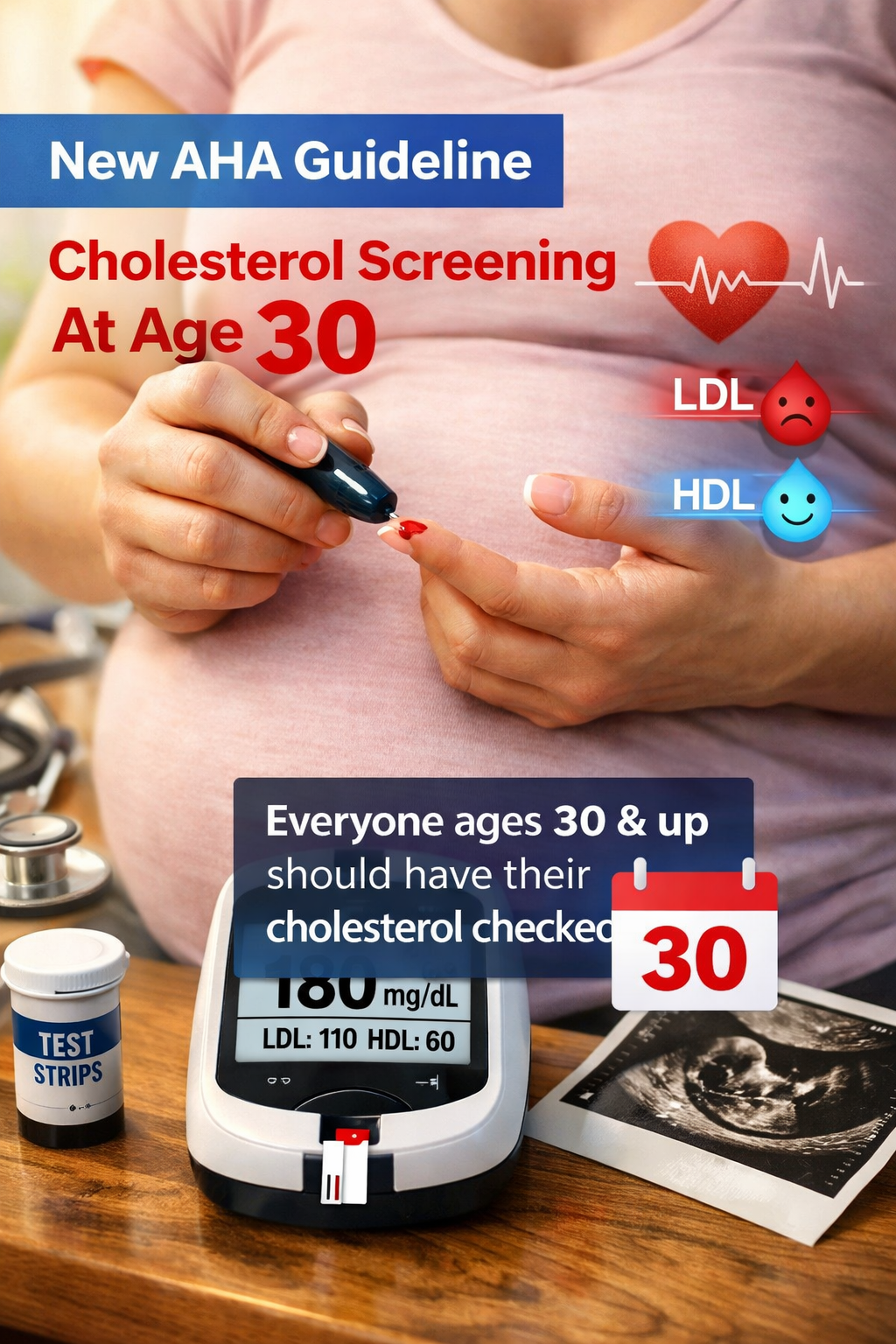
On March 13, 2026, the American Heart Association, the American College of Cardiology, and nine other medical societies updated the national cholesterol guidelines. The new directive: screen adults starting at age 30, using a calculator that estimates cardiovascular risk over 30 years, not just 10. The new LDL target for most adults 30 and older is below 100 mg/dL. The lead author said following these guidelines broadly could cut heart attack and stroke rates in half.
For preeclampsia survivors, this hits differently.
Preeclampsia and heart disease share the same biological roots: endothelial dysfunction, dyslipidemia, and inflammation. Women who had preeclampsia face twice the lifetime risk of heart disease and stroke, and four times the risk of heart failure. That risk begins building during pregnancy, often before anyone is watching cholesterol levels.
Yet fewer than 1 in 4 women with persistent hypertension after preeclampsia are referred to cardiology postpartum. What cholesterol test should follow every preeclampsia diagnosis? Rarely done.
The 2026 guidelines begin screening in the exact decade when people are having babies. Obstetric care and cardiovascular prevention are pointing at the same patient, and still not speaking to each other.
If you had preeclampsia, tell every provider. Ask for a lipid panel. Ask about your 30-year cardiovascular risk.
For clinicians: a preeclampsia diagnosis opens a cardiovascular file. It does not close at discharge.
The full clinical deep dive, mechanisms, data, and action steps at every stage of care — is on Pregnancy Blindspots on Substack.
The new guidelines moved the goalpost. Now the care has to catch up.
Want a deeper dive? Check out my Substack article